Article and image by Vince Giuliano
Stem cell injections have been shown to improve symptoms of Parkinson’s Disease (PD) in a rat model, essentially providing a “cure” for the disease. This is after 20 years of research on stem cell therapies for PD. When then will a stem cell therapy be available for PD in humans? In three or five years? I am quite sure the answer is no. More likely the answer is in 8-12 years if ever. This blog entry outlines progress so far and challenges yet to be faced. It also describes some of the challenges of translational medicine – getting successful treatments from the laboratory stage out to where they are part of clinical medicine. And it describes how some cell researchers seem to pay no attention to highly relevant findings of other stem cell researchers.
Background on Parkinson’s Disease
“Parkinson’s disease (also known as Parkinson disease, Parkinson’s, idiopathic parkinsonism, primary parkinsonism, PD, or paralysis agitans) is a degenerative disorder of the central nervous system. The motor symptoms of Parkinson’s disease result from the death of dopamine-generating cells in the substantia nigra, a region of the midbrain; the cause of this cell death is unknown. Early in the course of the disease, the most obvious symptoms are movement-related; these include shaking, rigidity, slowness of movement and difficulty with walking and gait. Later, cognitive and behavioural problems may arise, with dementia commonly occurring in the advanced stages of the disease. Other symptoms include sensory, sleep and emotional problems. PD is more common in the elderly, with most cases occurring after the age of 50. — 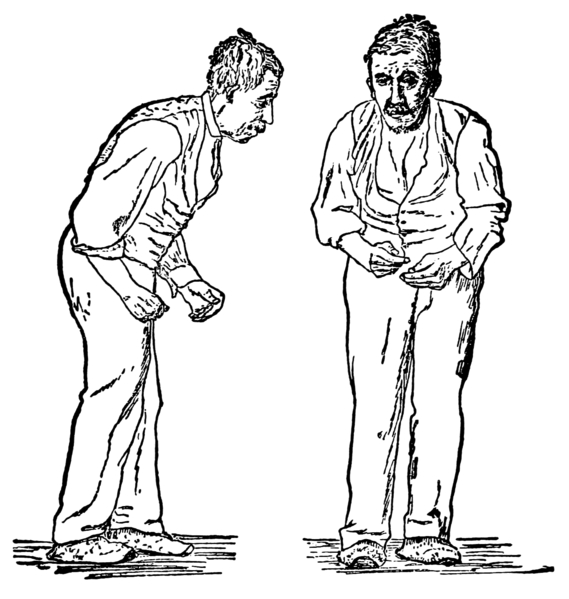 The main motor symptoms are collectively called
The main motor symptoms are collectively called
parkinsonism, or a “parkinsonian syndrome”. Parkinson’s disease is often defined as a parkinsonian syndrome that is idiopathic (having no known cause), although some atypical cases have a genetic origin(ref).”
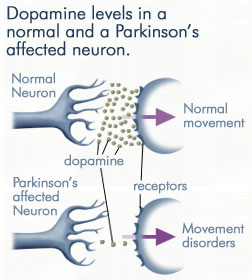
Availability of dopamine is essential for neurons involved in the coordination of body movements. For a complexity of reasons, PD results in the death of dopaminergic neurons. Symptoms of PD typically appear when 70% to 80% of the dopaminergic neurons are depleted.
The years have seen a steady increase in the number of publications related to PD and stem cells, and their relevancy. Literature links are established relating to the genetics of PD, to neuroinflammation and microglial activation in PD, to the role of oxidative damage and Nrf2 in PD, and to cell reprogramming factors required for adult brain neural stem cell differentiation into midbrain dopaminergic neurons. Fast forwarding to 2011 we start to see interesting results in the sciences involved and therapeutic experiments involving small animal models of PD. Most of the literature citations in this blog entry appeared during the last six months.
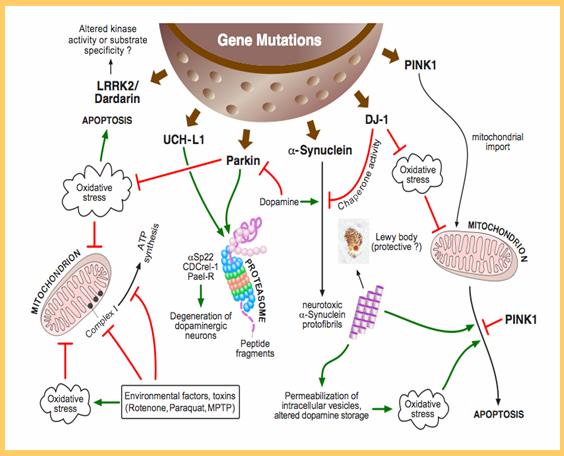
Gene mutations may be a cause for PD. Image source
There is still no cure for PD although drug and surgical treatments exist that can assist patients particularly in the earlier stages of the disease. Drugs used include deprenyl and levodopa and it is possible to surgically destroy the brain center that causes tremors. These treatments are all palliative and do not replace lost neurons nor stay the course of the disease.
Two of the major hopes for addressing PD are stem cell therapies and finding drugs that will slow or possibly reverse the course if the disease. This blog entry examines the first option. I have to a limited extent addressed the second option in the blog entry The pivotal role of Nrf2. Part 1 – a new view on the control of oxidative damage and generation of hormetic effects.
Parkinsons Disease and stem cell therapies
A Pubmed search on “stem cell therapy Parkinsons Disease” retrieves 945 research publications going back to 1968. The idea of transplanting neural stem cells as a therapy for PD seems to go back around 20 years, See Neural stem cells for CNS transplantation. (1993). The basic idea is deceptively simple. It is either 1.to transplant stem cells into the midbrain, the substantia nigra region, with the hope they reproduce and differentiate into dopamine-producing neurons to replace ones ravaged by PD, or 2.to use stem cells to generate quantities of dopamine-producing neurons and inject these instead..
Experiments in transferring dopamine-producing neurons into the midbrains of PD patients have been conducted since some 25 years ago.
The 2011 publication Dopamine cell transplantation for Parkinson’s disease: the importance of controlled clinical trialsreports: “Transplantation of human fetal dopamine neurons into the brain of Parkinson’s disease patients started in the late 1980s, less than 10 years after experiments in rats showed that embryonic dopamine neurons from a narrow window of development are suitable for transplantation. For human transplantation, the critical stage of development is 6 to 8 weeks after conception. Because putamen is the basal ganglia structure most depleted of dopamine in Parkinson’s disease and because it is the structure most closely mapped to the motor cortex, it has been the primary target for neurotransplantation. The double blind trial conducted at the University of Colorado, Columbia University, and North Shore University is the first controlled surgical trial performed in the field of neurosurgery. Results have shown that transplants of fetal dopamine neurons can survive transplantation without immunosuppression and without regard to the age of the patients. Transplants improved objective signs of Parkinson’s disease to the best effects of L-DOPA seen preoperatively. Placebo surgery produced no clinical changes. In subjects in whom transplants replaced the need for L-DOPA, the implants replicated the preoperative effects of L-DOPA, including dyskinesias in susceptible patients. Our trial has provided the first controlled evidence that dopamine cell transplants can improve the clinical state of patients with Parkinson’s disease.”
Researchers became hopeful that stem cells, with their ability to reproduce and differentiate into specific cell types like dopamine-producing neurons, would be a lot easier to collect than the fetal neurons and could do a better job.
Many researchers now feel clinical use of stem cells as a PD therapy in imminent. But some researchers thought the same thing 15 years ago.
The 1997 publication Neuronal cell transplantation for Parkinson’s and Huntington’s diseasesrelated: “The brain constitutes a privileged transplantation site. Under appropriate conditions neuronal tissues can survive transplantation into the damaged brain, integrate with the host, and alleviate functional impairments associated with neurological disease. The experimental techniques have been developed to the point of clinical application with demonstrable benefit in Parkinson’s disease, and similar applications in Huntington’s disease appear to be imminent. Nevertheless, present techniques require use of embryonic/fetal tissues which will limit the availability of donors for the foreseeable future. There is an active search for alternative sources of tissue that are equally effective but more readily available, including engineered cells, expanded stem/precursor cells, and xenografts.”
The umbrella concept of injecting stem cells into the midbrain as a therapy for PD includes a number of quite different possible approaches.
Decisions include:
- Whether the stem cell transplant is autologous (uses cells derived from cells of the same patient) or allogenic (uses cells derived from others, including “standardized” lines).
- The source and type of the stem cell, e.g., whether they are pluripotent stem cells from, embryonic or cord-blood tissue, are derived from iPSCs (cells epigenetically reverted to pluripotent status so they are like embryonic stem cells; see ref,ref,ref.), or are adult multipotent stem cells such as mesenchymal stem cells derived from bone marrow or adipose tissue.
- Whether and how to pay attention to stem cell senescence. There is good reason to suspect that many experiments in autologous stem cell transplantation for PD and other CNS diseases in elderly patients have been unsuccessful or only partially successful because the stem cells were senescent to start with. See the discussion in the recent blog entry Insights into the epigenetics and rejuvenation of adult stem cells – Improving prospects for extraordinary longevity. Even in most of the current publications discussed here, it seems few researchers pay any attention to the stem cell senescence issue which could well be critical.
Because there is so much possible variability in a stem cell therapy for PD, it is sometimes difficult to reconcile outcomes of related experiments or clinical trials.
Transplants of human neural stem cells into Parkinson Disease model rats can ameliorate both spontaneous motor behavior and cognitive performance.
The June 2012 publication Long term behavioral effects of functional dopaminergic neurons generated from human neural stem cells in the rat 6-OH-DA Parkinson’s disease model. Effects of the forced expression of BCL-X(L)reports: “Parkinson’s disease (PD) motor symptoms are caused by the progressive degeneration of ventral mesencephalic (VM) dopaminergic neurons (DAn) in the Substantia Nigra pars compacta (SNpc). Cell replacement therapy for PD is based on the concept that the implantation of DAn in the striatum can functionally restore the dopamine levels lost in the disease. In the current study we have used an immortalized human VM neural stem cell line (hVM1) that generates DAn with the A9 phenotype. We have previously found that the forced expression of Bcl-X(L) in these cells enhances DAn generation and improves, short-term, d-amphetamine-induced rotation after transplantation in the 6-OH-DA rat model of PD 2-month post-grafting. Since functional maturation of human A9 DAn in vivo requires long survival times, in the present study we investigated the behavioral amelioration induced by the transplantation of these precursors (naïve and Bcl-X(L)-modified) in the striatum of Parkinsonian rats for up to 5 months. The main findings observed are an improvement on drug-induced behaviour and importantly, in spontaneous behavior tests for both cell-transplanted groups. Finally, we have also tested whether the grafts could ameliorate cognitive performance in PD, in addition to motor deficits. Significant difference was observed for T-maze alternation test in the cell-transplanted animals as compared to sham operated ones. To our knowledge, this is the first report showing an amelioration in spontaneous motor behavior and in cognitive performance in Parkinsonian animals after receiving human VM neural stem cell grafts. Histological studies confirmed that the grafts generated mature dopaminergic cells.”
A large number of publications related to future clinical use of stem cells for PD therapies have appeared during the last six months. Many of these papers offer a cautiously optimistic outlook. Further, they tend to be redundant of one another, repeating more or less the same facts.
For example, the September 2011 publicationCell replacement therapy for Parkinson’s disease: how close are we to the clinic?reports:“Cell replacement therapy (CRT) offers great promise as the future of regenerative medicine in Parkinson´s disease (PD). Three decades of experiments have accumulated a wealth of knowledge regarding the replacement of dying neurons by new and healthy dopaminergic neurons transplanted into the brains of animal models and affected patients. The first clinical trials provided the proof of principle for CRT in PD. In these experiments, intrastriatal transplantation of human embryonic mesencephalic tissue reinnervated the striatum, restored dopamine levels and showed motor improvements. Sequential controlled studies highlighted several problems that should be addressed prior to the wide application of CRT for PD patients. Moreover, owing to ethical and practical problems, embryonic stem cells require replacement by better-suited stem cells. Several obstacles remain to be surpassed, including identifying the best source of stem cells for A9 dopaminergic neuron generation, eliminating the risk of tumor formation and the development of graft-induced dyskinesias, and standardizing dopaminergic cell production in order to enable clinical application. In this article, we present an update on CRT for PD, reviewing the research milestones, various stem cells used and tailored differentiation methods, and analyze the information gained from the clinical trials.”
Another example is the January 2012 publicationClinical application of stem cell therapy in Parkinson’s diseasewhichreports: “Cell replacement therapies in Parkinson’s disease (PD) aim to provide long-lasting relief of patients’ symptoms. Previous clinical trials using transplantation of human fetal ventral mesencephalic (hfVM) tissue in the striata of PD patients have provided proof-of-principle that such grafts can restore striatal dopaminergic (DA-ergic) function. The transplants survive, reinnervate the striatum, and generate adequate symptomatic relief in some patients for more than a decade following operation. However, the initial clinical trials lacked homogeneity of outcomes and were hindered by the development of troublesome graft-induced dyskinesias in a subgroup of patients. Although recent knowledge has provided insights for overcoming these obstacles, it is unlikely that transplantation of hfVM tissue will become routine treatment for PD owing to problems with tissue availability and standardization of the grafts. The main focus now is on producing DA-ergic neuroblasts for transplantation from stem cells (SCs). There is a range of emerging sources of SCs for generating a DA-ergic fate in vitro. However, the translation of these efforts in vivo currently lacks efficacy and sustainability. A successful, clinically competitive SC therapy in PD needs to produce long-lasting symptomatic relief without side effects while counteracting PD progression.”
Some review publications have tended to be on the less optimistic side when considering possible stem cell therapies for PD, focusing on issues yet to be resolved.
For example, the December 2011 E-pub Critical aspects of clinical trial design for novel cell and gene therapies. (Dec 2011)reports: “Neural cell transplantation and gene therapy have attracted considerable interest as promising therapeutic alternatives for patients with Parkinson’s disease (PD). Preclinical and open-label studies have suggested that grafted fetal neural tissue or viral vector gene transfer can achieve considerable biochemical and clinical improvements, whereas subsequent double-blind, placebo-controlled protocols have produced rather more modest and variable results. Detailed evaluation of these discordant findings has highlighted several crucial issues such as patient selection criteria, details surrounding transplantation or gene therapy methodologies, as well as the study designs themselves that ought to be carefully considered in the planning phases of future clinical trials. Beyond the provision of symptomatic efficacy and safety data, it also remains to be identified whether the possibilities offered by stem cell and gene therapy technological advances might translate to meaningful neuroprotection and/or disease-modifying effects or alleviate the nonmotor aspects of PD and thus offer additional benefits beyond those achieved through conventional pharmacotherapy or deep brain stimulation (DBS).”
Many researchers have seen hope for a PD therapy based on allogenic transplantation of mesenchymal stem cells. In a pilot clinical trial. transplantation of allogenic mesenchymal stem cells provided limited improvements in early-stage PD patients.
The March 2012 E-publication Bilateral transplantation of allogenic adult human bone marrow-derived mesenchymal stem cells into the subventricular zone of Parkinson’s disease: a pilot clinical studyreports: “The progress of PD and its related disorders cannot be prevented with the medications available. In this study, we recruited 8 PD and 4 PD plus patients between 5 to 15 years after diagnosis. All patients received BM-MSCs bilaterally into the SVZ and were followed up for 12 months. PD patients after therapy reported a mean improvement of 17.92% during “on” and 31.21% during “off” period on the UPDRS scoring system. None of the patients increased their medication during the follow-up period. Subjectively, the patients reported clarity in speech, reduction in tremors, rigidity, and freezing attacks. The results correlated with the duration of the disease. Those patients transplanted in the early stages of the disease (less than 5 years) showed more improvement and no further disease progression than the later stages (11-15 years). However, the PD plus patients did not show any change in their clinical status after stem cell transplantation. This study demonstrates the safety of adult allogenic human BM-MSCs transplanted into the SVZ of the brain and its efficacy in early-stage PD patients.”
Oxidative damage coupled with activated microglia are thought to contribute to a vicious cycle in the substantia nigra of the midbrain region leading to loss of as well as lack of replacement of dopaminergic neurons. Given this aetiology of PD, the optimal strategy for treating PD may involve combining upgrading of expression of Nrf2 with mesenchymal or some other stem cell therapy.
This is my hypothesis.
One leg supporting this hypothesis is the July 2012 publication Can mesenchymal stem cells reduce vulnerability of dopaminergic neurons in the substantia nigra to oxidative insult in individuals at risk to Parkinson’s disease? which reports: “PD (Parkinson’s disease) is characterized by the selective loss of DA (dopaminergic) neurons in the substantia nigra of the midbrain region, but not in the ventral tegmental area and other catecholaminergic cell group areas. The aetiology of PD is attributed both to environmental and genetic causes, and certain population of individuals may be classified as at risk of developing PD later in life. However, there are as yet no therapy regimens that can help to delay or prevent the onset of the disease to realize long-term benefits from this early diagnosis. In PD, a vicious cycle gets initiated in the substantia nigra, because of which susceptible neurons continue to degenerate whereas damaged neurons do not get enough support for regeneration. This happens primarily because of the local environment of oxidative damage brought about by the dual presence of dopamine and high levels of iron, decline in cellular detoxification systems and low density of glial cells surrounding the DA neurons in the mesencephalic region. To enhance the defence mechanism of the substantia nigra in this situation, it is necessary to combat the oxidative insult while providing trophic factors for the survival and regeneration of the damaged neurons. In light of in vitro and in vivo studies, MSCs (mesenchymal stem cells) as candidates for cell-based therapies in PD have greater scope than as mere replacement of cell type, since they can be used as a cellular system for the detoxification of ROS (reactive oxygen species) as well as a supplier of neurotrophic factors to modulate the local environment. Building on progress in unravelling the multipronged effect of MSCs, we therefore hypothesize that MSCs could be used as a prophylactic strategy to delay or prevent the onset of PD in at-risk individuals, and to slow down the progression of the disease.”
The other leg supporting the hypothesis is the section Nrf2 and Parkinson’s disease in the blog entry The pivotal role of Nrf2. Part 1 – a new view on the control of oxidative damage and generation of hormetic effects.
Further supporting the use of mesenchymal stem cells for PD therapy is the February 2012 E-publicationParkinson’s disease and mesenchymal stem cells: potential for cell-based therapy. “Cell transplantation is a strategy with great potential for the treatment of Parkinson’s disease, and many types of stem cells, including neural stem cells and embryonic stem cells, are considered candidates for transplantation therapy. Mesenchymal stem cells are a great therapeutic cell source because they are easy accessible and can be expanded from patients or donor mesenchymal tissues without posing serious ethical and technical problems. They have trophic effects for protecting damaged tissues as well as differentiation ability to generate a broad spectrum of cells, including dopamine neurons, which contribute to the replenishment of lost cells in Parkinson’s disease. This paper focuses mainly on the potential of mesenchymal stem cells as a therapeutic cell source and discusses their potential clinical application in Parkinson’s disease.”
Scalable techniques are known for creating inducing iPSC cells to differentiate onto engraftable dopamine-expressing neurons. Further, such neurons can successfully engraft in mice, rats and monkeys.
The November 2011 publication Dopamine neurons derived from human ES cells efficiently engraft in animal models of Parkinson’s disease. reports: “Human pluripotent stem cells (PSCs) are a promising source of cells for applications in regenerative medicine. Directed differentiation of PSCs into specialized cells such as spinal motoneurons or midbrain dopamine (DA) neurons has been achieved. However, the effective use of PSCs for celltherapy has lagged behind. Whereas mouse PSC-derived DA neurons have shown efficacy in models of Parkinson’s disease, DA neurons from human PSCs generally show poor in vivo performance. There are also considerable safety concerns for PSCs related to their potential for teratoma formation or neural overgrowth. Here we present a novel floor-plate-based strategy for the derivation of human DA neurons that efficiently engraft in vivo, suggesting that past failures were due to incomplete specification rather than a specific vulnerability of the cells. Midbrain floor-plate precursors are derived from PSCs 11 days after exposure to small molecule activators of sonic hedgehog (SHH) and canonical WNT signalling. Engraftable midbrain DA neurons are obtained by day 25 and can be maintained in vitro for several months. Extensive molecular profiling, biochemical and electrophysiological data define developmental progression and confirm identity of PSC-derived midbrain DA neurons. In vivo survival and function is demonstrated in Parkinson’s disease models using three host species. Long-term engraftment in 6-hydroxy-dopamine-lesioned mice and rats demonstrates robust survival of midbrain DA neurons derived from human embryonic stem (ES) cells, complete restoration of amphetamine-induced rotation behaviour and improvements in tests of forelimb use and akinesia. Finally, scalability is demonstrated by transplantation into parkinsonian monkeys. Excellent DA neuron survival, function and lack of neural overgrowth in the three animal models indicate promise for the development of cell-based therapies in Parkinson’s disease.”
Although significant progress has been made in creating a process for manufacturing dopaminergic neurons from stem cells, it may still take a long additional time before such neurons can be used as a PD therapy in clinical practice.
In a Buck Institute community seminar available on video The Future Of Regenerative Medicine: What’s Aging Got To Do With It?(May 2012), Buck staff researcher.Xianmin Zeng gives a short talk on Stem Cells for Treating Disease and Drug Discovery, a talk worth watching. In this presentation, Dr. Zeng points out that steps to creating such a therapy are as below. Comment in parentheses and italics are mine:
- Create stem cell lines that are suitable for clinical use (Many stem cell lines, including commercial iPSC lines, may be suitable for drug screening but do not meet safety criteria for human use. For example, they might contain oncogenic genes from the viral vector used in the cell reversion process. See below for additional comments in iPSCs.)
- Produce the right type of neuron (dopaminergic neuron) from stem cells. (The previously-mentioned publication indicates that this step and the next step appear to be feasible.)
- Manufacture dopaminergic neurons in a GMP (Good medical Practice) facility suitable for clinical trials. (It is one thing to produce small quantities of dopaminergic neurons in a laboratory. It is a second thing requiring different technology to manufacture such neurons in quantity ensuring purity of strain. And it is a third thing to do this under conditions that ensure safety of the resulting product for clinical use Dr. Zeng reports that she and her colleagues have established a well-characterized GMP-compatible and scalable 4- step process for generating dopaminergic neurons. In other words they have gotten to the point where they have engaged a partner organization for manufacturing.)
- Evaluate efficacy, safety and the requirement for immune suppression in suitable animal models. (Yes but tricky since the requirements for humans may be different than those for lab animals.)
- Design a clinical trial protocol. Assemble an IND application. (We know that starting at this point, the process through a successful Phase 3 clinical trial can easily by itself take 8 or more years.)
(Dr. Zeng is here outlining only one of several possible ways to proceed. She is thinking about manufacturing large quantities of dopaminergic neurons which will be administered allogenically. This is a very different process than injecting stem cells into humans with the hope they will differentiate in-vivo into dopaminergic neurons, a process that could be done autologously avoiding immune system rejection issues. Supporting this approach, Dr. Zeng points out that the cells produced by this process “cured” PD in rats. Working with various partner organizations, Dr. Zeng and her associates are now simultaneously working on stage 3, 4, and 5 of the above process. How long before entering human clinical trials is unclear. In addition to the concern about immune rejection, I think there may be another issue connected with cell senescence. For example, if the dopaminergic neurons manufacturing process requires a significant number of replicative passages, this could contribute to the resulting crop of dopaminergic neurons being epigenetically old, nearing senescence. I see the senescence issue as key and discuss it further below,)
Immune system rejection continues to be an issue in pre-clinical animal models for evaluating allogenic stem cell therapies for PD.
The problem of course applies to allogenic grafts (transfers where the donor animal is different than the recipient animal) of all kinds. The June 2012 publication INTRACEREBRAL TRANSPLANTATION OF DIFFERENTIATED HUMAN reports: “To explore stem celltherapy for Parkinson’s disease (PD), three adult rhesus monkeys were first rendered hemi-parkinsonian by unilateral intracarotid 1-methyl-4-phenyl-1,2,3,6- tetrahydropyridine (MPTP) infusion. Five months post-infusion, they were given MRIguided stereotaxic intrastriatal and intranigral injections of green fluorescent protein (GFP)- labeled cultures of dopaminergic neurons derived from human embryonic stem cells (DA-hES cells). The animals were immunosuppressed using daily oral cyclosporine (CsA). Three months later, viable grafts were observed at the injection sites in one animal while no obvious grafts were present in the other two monkeys. The surviving grafts contained numerous GFPpositive cells that were positively labeled for nestin and MAP2 but not for glial fibrillary acidic protein (GFAP), NeuN, or tyrosine hydroxylase (TH). The grafted areas in all animals showed dense staining for GFAP, CD68, and CD45. These results indicated that xenografts of human stem cell derivatives in CsA-suppressed rhesus brain were mostly rejected. Our study suggests that immunological issues are obstacles for preclinical evaluation of hES cells and that improved immunosuppression paradigms and/or alternative cell sources that do not elicit immune rejection are needed for long-term preclinical studies.”
For PD therapy, induced pluripotent stem cells (iPSCs) have perhaps the greatest potentiality because they can be used autologously avoiding immune rejection issues, because their differentiation can be effectively directed and because they are free of epigenetic senescence markers. Yet despite much progress over five years now, safety and suitability of these cells for human use remains in question.
The April 2012 publication Human induced pluripotent stem cells and neurodegenerative disease: prospects for novel therapiesprovides an overview of stem cell treatments for PD and other degenerative neurological disorders: “PURPOSE OF REVIEW: The lack of effective treatments for various neurodegenerative disorders has placed huge burdens on society. We review the current status in applying induced pluripotent stem cell (iPSC) technology for the cellular therapy, drug screening, and in-vitro modeling of neurodegenerative diseases. RECENT FINDINGS: iPSCs are generated from somatic cells by overexpressing four reprogramming factors (Oct4, Sox2, Klf4, and Myc). Like human embryonic stem cells, iPSCs have features of self-renewal and pluripotency, and allow in-vitro disease modeling, drug screening, and cell replacement therapy. Disease-specific iPSCs were derived from patients of several neurodegenerative diseases, including Parkinson’s disease, Alzheimer’s disease, amyotrophic lateral sclerosis, and spinal muscular atrophy. Neurons differentiated from these iPSCs recapitulated the in-vivo phenotypes, providing platforms for drug screening. In the case of Parkinson’s disease, iPSC-derived dopaminergic neurons gave positive therapeutic effect on a rodent Parkinson’s disease model as a proof of principle in using iPSCs as sources of cell replacement therapy. Beyond iPSC technology, much effort is being made to generate neurons directly from dermal fibroblasts with neuron-specific transcription factors, which does not require making iPSCs as an intermediate cell type. SUMMARY: We summarize recent progress in using iPSCs for modeling the progress and treatment of neurodegenerative diseases and provide evidence for future perspectives in this field.”
A case for use of iPSCs in therapies for PD is made in the April 2012 publication Stem celltherapy ameliorates bladder dysfunction in an animal model of Parkinson disease: “Parkinson’s disease has been so far commonly treated with medication therapy. Although the medication works effectively in the initial phase, it turns out to be less effective at the later stage of the disease. Recently, induced pluripotent stem (iPS) cells have attracted much attention because of their potential to cure diseases such as Parkinson’s disease. Due to the accumulating clinical experiences of cell transplantation procedures with aborted fetal tissues, Parkinson’s disease has become one of the most promising targets for the clinical application of this iPS cell technology. In this review, we will summarize the ongoing research in the field of iPS cells and Parkinson’s disease. The method for establishing iPS cells has advanced rapidly that can be applied in the clinical stage in terms of avoiding the use of viral vectors, xenogenic materials, etc. The differentiation protocol to derive the dopamine neurons from iPS cells has also been improved. However, several issues, such as the risk of tumor formation and the poor survival of the grafted dopamine neurons in vivo remain to be solved before these cells can be used in the clinical settings. Other than cell transplantations, iPS cell technology can also provide a valuable platform for disease analysis and drug development with in vitro systems of human cells. Several lines of iPS cells have already been established from Parkinson’s disease patients with either sporadic or genetic background. For patients to achieve maximum benefits of this technology, further research must be conducted in both fields, that is, cell transplantation and the disease modeling with patient-derived iPS cells.”
An optimistic projection for combining iPSC or other approaches to cell reprogramming with other therapies for PD is set forward in the April 2012 publication Progress on stem cell research towards the treatment of Parkinson’s disease. “Parkinson’s disease (PD) is a neurodegenerative disorder characterized by the progressive accumulation of Lewy body inclusions along with selective destruction of dopaminergic (DA) neurons in the nigrostriatal tract of the brain. Genetic studies have revealed much about the pathophysiology of PD, enabling the identification of both biomarkers for diagnosis and genetic targets for therapeutic treatment, which are evolved in tandem with the development of stem cell technologies. The discovery of induced pluripotent stem (iPS) cells facilitates the derivation of stem cells from adult somatic cells for personalized treatment and thus overcomes not only the limited availability of human embryonic stem cells but also ethical concerns surrounding their use. Non-viral, non-integration, or non-DNA-mediated reprogramming technologies are being developed. Protocols for generating midbrain DA neurons are undergoing constant refinement. The iPS cell-derived DA neurons provide cellular models for investigating disease progression in vitro and for screening molecules of novel therapeutic potential and have beneficial effects on improving the behavior of parkinsonian animals. Further progress in the development of safer non-viral/non-biased reprogramming strategies and the subsequent generation of homogenous midbrain DA neurons shall pave the way for clinical trials. A combined approach of drugs, cell replacement, and gene therapy to stop disease progression and to improve treatment may soon be within our reach.”
About a year ago, the general outlook for using iPSCs as part of a clinical approach to treating PD seemed to be more negative, although many of the challenges connected with human use if iPSCs identified then remain now.
For example, the July 2011 publication UNCERTAIN TRANSLATION, UNCERTAIN BENEFIT AND UNCERTAIN RISK: ETHICAL CHALLENGES FACING FIRST-IN-HUMAN TRIALS OF INDUCED PLURIPOTENT STEM (IPS) CELLS reports: “The discovery of induced pluripotent stem (iPS) cells in 2006 was heralded as a major breakthrough in stem cell research. Since then, progress in iPS cell technology has paved the way towards clinical application, particularly cell replacement therapy, which has refueled debate on the ethics of stem cell research. However, much of the discourse has focused on questions of moral status and potentiality, overlooking the ethical issues which are introduced by the clinical testing of iPS cell replacement therapy. First-in-human trials, in particular, raise a number of ethical concerns including informed consent, subject recruitment and harm minimisation as well as the inherent uncertainty and risks which are involved in testing medical procedures on humans for the first time. These issues, while a feature of any human research, become more complex in the case of iPS celltherapy, given the seriousness of the potential risks, the unreliability of available animal models, the vulnerability of the target patient group, and the high stakes of such an intensely public area of science. Our paper will present a detailed case study of iPS cell replacement therapy for Parkinson’s disease to highlight these broader ethical and epistemological concerns. If we accept that iPS cell technology is fraught with challenges which go far beyond merely refuting the potentiality of the stem cell line, we conclude that iPS cell research should not replace, but proceed alongside embryonic and adult somatic stem cell research to promote cross-fertilisation of knowledge and better clinical outcomes.”
The December 2011 publication Clinical translation of cell transplantation in the brainconcludes:” In spite of rapid progress, the conditions for reliable, well tolerated and effective cell therapies in brain disease are not yet fully established.”
iPSCs provide very useful models for testing PD therapies.
About this there is no conflict. The June 2012 publication Modeling Parkinson’s disease using induced pluripotent stem cells reports: “Our understanding of the underlying molecular mechanism of Parkinson’s disease (PD) is hampered by a lack of access to affected human dopaminergic (DA) neurons on which to base experimental research. Fortunately, the recent development of a PD disease model using induced pluripotent stem cells (iPSCs) provides access to cell types that were previously unobtainable in sufficient quantity or quality, and presents exciting promises for the elucidation of PD etiology and the development of potential therapeutics. To more effectively model PD, we generated two patient-derived iPSC lines: a line carrying a homozygous p.G2019S mutation in the leucine-rich repeat kinase 2 (LRRK2) gene and another carrying a full gene triplication of the α-synuclein encoding gene, SNCA. We demonstrated that these PD-linked pluripotent lines were able to differentiate into DA neurons and that these neurons exhibited increased expression of key oxidative stress response genes and α-synuclein protein. Moreover, when compared to wild-type DA neurons, LRRK2-G2019S iPSC-derived DA neurons were more sensitive to caspase-3 activation caused by exposure to hydrogen peroxide, MG-132, and 6-hydroxydopamine. In addition, SNCA-triplication iPSC-derived DA neurons formed early ubiquitin-positive puncta and were more sensitive to peak toxicity from hydrogen peroxide-induced stress. These aforementioned findings suggest that LRRK2-G2019S and SNCA-triplication iPSC-derived DA neurons exhibit early phenotypes linked to PD. Given the high penetrance of the homozygous LRRK2 mutation, the expression of wild-type α-synuclein protein in the SNCA-triplication line, and the clinical resemblance of patients afflicted with these familial disorders to sporadic PD patients, these iPSC-derived neurons may be unique and valuable models for disease diagnostics and development of novel pharmacological agents for alleviation of relevant disease phenotypes.”
Cell senescence, particularly stem cell senescence, appears to be a largely ignored issue in the literature connected with PD stem cell treatments, but it could be a crucial one explaining many of the mixed results obtained to date.
For example, I note that 1. Allogenic mesenchymal stem cell transplantation though much-focused on has so far produced at best mixed results with humans. 2. In the papers on mesenchymal stem cell transplantation for PD, I have not come across any discussion of stem cell senescence. The issue appears to be invisible to the researchers. 3. Yet, other researchers than those involved in PD transplantation point out that transplants involving senescent stem cells are unlikely to work(ref).
Adult stem cells, like dopaminergic neurons and all other normal body cell types, undergo a process of epigenetic changes and accumulation of DNA damage as an animal ages, culminating at advanced age with senescent stem cells that can no longer readily differentiate into somatic cell types. The process starts at conception. Therefore, transplants of mesenchymal or other adult stem cells from an aged healthy donor can be a transplant of cells well on their way to senescence and non-functionality. And this is true whether the donor is the animal receiving the transplant or another.
Reverting cells to iPSC status as a stage in the transplantation process restores the cells epigenetic age markers to a youthful state (that essentially of embryonic stem cells), obviating the problem of aged donor cells. However, even in that case, if the cells are forced to replicate many time outside the body as part of a manufacturing process, this process alone leads the resulting cells down the road to senescence. This is true if the manufacturing involves replication of either adult stem cells or body cells like dopaminergic neurons.
For amplification of some these points, please see my recent blog entry Insights into the epigenetics and rejuvenation of adult stem cells – Improving prospects for extraordinary longevity.
The issue of high variability among donor cells and age of donors are raised in this July 2012 publication, but without reference to the central issue of cell senescence: Birth dating of midbrain dopamine neurons identifies A9 enriched tissue for transplantation into Parkinsonian mice. “Clinical trials have provided proof of principle that new dopamine neurons isolated from the developing ventral midbrain and transplanted into the denervated striatum can functionally integrate and alleviate symptoms in Parkinson’s disease patients. However, extensive variability across patients has been observed, ranging from long-term motor improvement to the absence of symptomatic relief and development of dyskinesias. Heterogeneity of the donor tissue is likely to be a contributing factor in the variable outcomes. Dissections of ventral midbrain used for transplantation will variously contain progenitors for different dopamine neuron subtypes as well as different neurotransmitter phenotypes. The overall impact of the resulting graft will be determined by the functional contribution from these different cell types. The A9 substantia nigra pars compacta dopamine neurons, for example, are known to be particularly important for motor recovery in animal models. Serotonergic neurons, on the other hand, have been implicated in unwanted dyskinesias. Currently little knowledge exists on how variables such as donor age, which have not been controlled for in clinical trials, will impact on the final neuronal composition of fetal grafts. Here we performed a birth dating study to identify the time-course of neurogenesis within the various ventral midbrain dopamine subpopulations in an effort to identify A9-enriched donor tissue for transplantation. The results show that A9 neurons precede the birth of A10 ventral tegmental area dopamine neurons. Subsequent grafting of younger ventral midbrain donor tissue revealed significantly larger grafts containing more mitotic dopamine neuroblasts compared to older donor grafts. These grafts were enriched with A9 neurons and showed significantly greater innervation of the target dorso-lateral striatum and DA release. Younger donor grafts also contained significantly less serotonergic neurons. These findings demonstrate the importance of standardized methods to improve cell therapy for Parkinson’s disease and have significant implications for the generation and selectivity of dopamine neurons from stem cell based sources.” The italics here highlighting the importance of donor youth and the relevance of cell senescence are my own.
Given that I have seen no direct discussion of this senescence issue in the publications of those concerned with stem cell therapies for PD, It is tempting to infer that the knowledge bases of some current researchers are too old and/or too narrow for what they want to accomplish. Senescence of stem cells is a hot new topic, highly relevant to those who want to use stem cell transplants.
A large number of other potentially relevant publications have appeared in the last year. They include:
Potential role of α-synuclein in neurodegeneration: studies in a rat animal model. (May 2012)
Stromal factors SDF1α, sFRP1, and VEGFD induce dopaminergic neuron differentiation of human pluripotent stem cells. (E-pub April 2012)
Parkinsons Disease and mesenchymal stem cells: potential for cell-based therapy. (Epub 2012 Feb 28)
Stem cell challenges in the treatment of neurodegenerative disease. (2011)
Wrapping it up
First a caution related to the idea that cell replacement therapy might cure PD. Loss of dopamine-producing neurons is a downstream effect of the disease that is caused by other processes. So, simply replacing such lost neurons via stem cells does not address those other processes and may turn out to be useful but is not a cure, just like dopamine-replacement via taking levodopa does not constitute a cure. If, on the other hand, microglial or neural stem cell senescence is a root cause of PD, then it is possible that replacement of senescent stem cells with epigenetically young ones could bring about a real cure.
Still, I join the chorus in thinking that one or more effective stem cell therapies for PD will enter the clinic. Together with other new interventions such as selective activation of Nrf2, such a therapy will serve, at best, effectively to “cure” the PD disease, at worst to effectively halt its progression.
Given all the factors discussed here I estimate 8-12 years time will be required before anything approaching a stem cell “cure” for PD will be widely available in the clinic. Perhaps even more.
Researchers and clinicians concerned with cell-replacement therapies for PD and other neurological disease should start paying attention to the growing body of knowledge on stem cell aging and senescence. This might significantly speed up the historical trial-and-error process aimed at finding a cure.



Nice article. Stem cell therapy is good to cure Parkinson’s disease. Stem cell therapy helps to protect brain cells. Parkinson disease is the brain disorder that can cause memory loss, damage brain cells etc. There are many anti aging treatment available to treat Alzheimer’s disease and Parkinson’s disease.
Pingback: Diabetes Parkinson’s Disease Cure Close | Diabetes Reversed